Cardiogenic Shock and Intraortic Balloon Pump CVS029
Cardiogenic Shock and Intraortic Balloon Pump Transcript
Cardiogenic Shock and Intraortic Balloon Pump
This is Dr. Cal Shipley with a review of intraaortic balloon pump usage in myocardial infarction with cardiogenic shock.
Myocardial Infarction
Myocardial infarction, also known as heart attack, occurs due to disease in coronary arteries, which impairs blood flow to the heart muscle (also known as the myocardium). Impaired coronary artery blood flow results in decreased delivery of oxygen and nutrients to the myocardium. If the loss of oxygen and nutrient flow reaches critical levels, a myocardial infarction occurs.
The term myocardial infarction means death of cardiac muscle. Because it has the greatest workload of the cardiac chambers, the left ventricle has the largest demand for oxygen and nutrients, and therefore, is most commonly involved in myocardial infarction. While infarction may occur anywhere within the left ventricular musculature, the apex of the ventricle (as shown here) is a commonly involved area. The dead muscle in the area of infarction no longer contracts. Cardiac output is reduced, and this reduction in output is directly proportional to the size of the infarct. If the area of the infarct is large enough, cardiac output may be critically reduced, resulting in significant loss of blood flow to all bodily organs and tissues.
Cardiogenic Shock
This is known as cardiogenic shock. Viewed from the patient’s left side, the effect of a significant infarct on left ventricular contraction is apparent. The effect of the infarct on left ventricular function is further amplified by the fact that with reduced cardiac output, there is also reduced flow through the coronary arteries. This sets up a vicious cycle which may result in extension of the infarcted area, a situation which, if not corrected rapidly, may lead to ventricular arrhythmias such as ventricular tachycardia, or ventricular fibrillation, and ultimately, cardiac arrest and death.
Intraortic Balloon Pump
In such situations, placement of an intra-aortic balloon pump may break the vicious cycle and stabilize cardiac function. Let’s return again to our cross-sectional view of the infarcted left ventricle, viewed from the patient’s left side. The balloon pump is typically inserted via the left or right femoral artery in the groin and then advanced into the upper aorta in position such that the end of the balloon is a couple of centimeters away from the origin of the left subclavian artery in the aortic arch. The balloon is capable of being inflated or deflated.
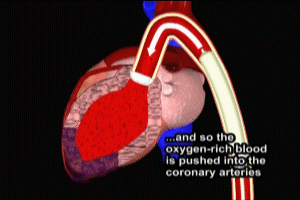
During systole, the balloon is deflated. This creates suction within the aortic root, which draws blood into the aorta, increasing cardiac output and reducing the workload of the left ventricle. Cardiac output is increased, and so is flow to the coronary arteries. During diastole, the balloon is inflated. This creates positive pressure within the aorta, pushing blood back towards the left ventricle. Because the aortic valve is closed during diastole, the blood is pushed into the coronary arteries, further improving flow to the myocardium.
The combination of improved coronary blood flow and increased cardiac output with decreased left ventricular workload is enough to stabilize many patients with myocardial infarction and cardiogenic shock. The inflation and deflation of the balloon pump is synchronized with the cardiac cycle via an external electronic module which is typically attached to an electrocardiogram unit, or a pressure transducer in the tip of the balloon. The synchronized inflation and deflation of the balloon pump is known as counterpulsation. Helium gas is used for inflation as it has a low viscosity and moves rapidly through the extended tubing attached to the balloon. It is also less likely than air to embolize should the balloon rupture.
It’s important to note that the intraaortic balloon pump is a temporary measure. It may be left in place for up to several days.
Cal Shipley, MD. copyright 2020