The Appendix Transcript
The Appendix
This is Dr. Cal Shipley with a review of the appendix: anatomy, physiology, and acute appendicitis.
Anatomy of the Appendix
Let’s start by taking a look at the anatomy and physiology of the normal appendix.
The appendix is located in the right lower quadrant of the abdomen just below the junction of the ileum and the colon.
The appendix projects from the most proximal portion of the colon known as the cecum. It is formally designated as the vermiform appendix. Vermiform is the Latin word for “worm-like”.
Blood Supply
Attached to the appendix along its inner or medial border is a fibro-fatty piece of tissue known as the mesoappendix. Within the mesoappendix runs the blood supply to the appendix, the appendiceal artery. Of note is the fact that the appendiceal artery is not simply a tributary of arteries feeding the colon, but has its own origin from the ileocolic artery.
Size and Location
The length of the appendix can vary from 2 centimeters (about an inch) up to 20 centimeters, (about 8 inches) with an average length of 9 centimeters (about 3 inches).
Typically, the base of the appendix is attached to the cecum at a point about one inch below the ileocecal valve, which is located at the previously mentioned junction between the ileum and the colon.
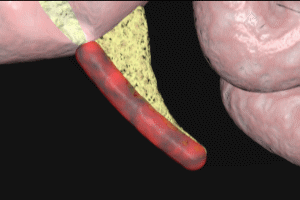
While the position of the base of the appendix varies very little from individual to individual, the course of its distal portion is quite variable, with approximately one third pointing over the brim of the pelvis (as shown here), 65% retrocecal, that is, running behind the cecum, and a small percentage pointing towards the ileum and running in front (anterior to it); pointing towards the ileum, and running behind (posterior) to it; and pointing down to the right.
While the positions depicted here comprise the majority of those seen, virtually any direction from the base is possible.
McBurney’s Point
In 1889, an American surgeon who had a special interest in appendicitis, Dr. Charles McBurney, described a point approximately one-third of the way along a line drawn from the anterior superior iliac spine to the umbilicus as being the point of maximum tenderness in patients with acute appendicitis. Thereafter, this area became known as McBurney’s point.
The Peritoneum
Most of the stomach, the small intestine, the liver, and the colon, including the appendix, are enclosed in a membrane known as the peritoneum.
Here is a cross-sectional view looking from the side at the peritoneal membrane in dark blue, and the organs that it encloses, including the appendix, noted near the bottom of the image.
The Appendix in Early Man
The precise role of the appendix in human physiology has been debated for a hundred years. What is generally agreed upon is that it is a vestigial structure, that is, an organ which had a particular purpose early in the development of mankind and whose function was no longer required as the human body evolved.
One fascinating theory is that the cecum was once much larger than in its current form, and that it served as a large pouch to aid in the digestion of the highly plant-based diet of early man.
Over the course of millions of years, as agricultural technology was developed providing for more digestible foods, the large pouch-like cecum became redundant and shrank to its current size, leaving the small appendix as a vestige of the former pouch. This theory is not completely without foundation in that several mammal species alive today, such as horses, have an extended cecum which functions as an aid to digestion.
Role of the Appendix in Modern Humans
All of this begs the question, does the appendix have any contributory role in current human physiology? For decades, the appendix was considered a useless appendage, a leftover from our evolutionary past. It’s removal from the body did not appear to have any adverse consequences.
As a result of this outlook, surgeons often removed normal appendixes in the course of other pelvic and lower abdominal surgeries to eliminate the possibility of appendicitis in the future. In recent years, that thinking has begun to change.
Structure of the Appendix
To better understand this, let’s take a closer look at the structure of the appendix.
Let’s zoom in on the appendix and take a look at it in cross-section.
And closer yet to see a microscopic view. Here we see the inner channel, or lumen, of the appendix, and in cross-section, the wall, with its innermost component, the mucosa. Unlike the small intestine which contains numerous finger-like projections known as villi, which increase the surface area for absorption of nutrients, the mucosal lining of the appendix is similar to that of the colon, consisting primarily of a single cell layer of columnar epithelium.
Blood supply to the mucosa is provided by capillaries as shown. Let’s zoom in for a closer look. On closer inspection of the mucosa, the individual columnar epithelial cells are more apparent. Periodic gaps or crypts, known as the crypts of Lieberkuhn, are lined by columnar epithelium cells interspersed with goblet cells, so named for their resemblance to drinking goblets. The goblet cells produce mucus, which flows up and out of the crypts. The mucus provides a protective coating to the mucosal layer, and also helps to sweep away foreign material and dead epithelial cells.
Stem cells located in the bases of the crypts generate new epithelial cells when needed.
Lymphoid Aggregates
Contained within the appendiceal wall, below the mucosa layer, are the key to the contributory role of the appendix in current human physiology: aggregations of lymphoid tissue. These aggregates are present throughout the appendix, and recent research has demonstrated that they contribute to both gut and systemic immune defenses. The lymphoid tissue assists in the maturation of B lymphocyte white blood cells, as well as aiding the production of IgA antibodies, both of which are then available to enter the circulatory system, and hence, travel to anywhere in the body.
Researchers have also shown that the appendiceal lymphoid tissue is involved in the production of chemicals which help to direct the movement of lymphocytes to other parts of the body.
Local Immunity in the Gut
At the gut level, the appendix appears to contribute to local immunity by sensitizing white blood cells to the various antigens in foreign substances present within the gastrointestinal tract. What role these various immune functions of the appendix may play in the development of chronic inflammatory bowel diseases, such as Crohn’s disease or ulcerative colitis, is as yet unknown.
Commensal Bacteria
Another interesting area of research into the role of the appendix in modern human physiology involves bacteria. The appendix has been found to contain abundant, helpful bacteria also known as commensal bacteria.
Commensal bacteria play several important roles in the human gut, including assistance with digestion and absorption of nutrients, maintenance of intestinal architecture, stimulation of the immune system, and suppression of pathogenic bacteria through nutrient competition. [silence] One recent study of hospitalized patients, all of whom had had previous infections with Clostridium difficile, demonstrated that those who had previously had appendectomies were four times more likely to have recurrent C. difficile infection. It has been proposed then that the appendix may act as a reservoir for commensal bacteria ready to replenish the gut microflora when depleted by pathogenic infection or other illness.
In summary, whatever role the appendix played in ancient human physiology, recent research has shown that it clearly has a significant role to play in modern humankind both in support of gut and systemic immune defense. As a result of this very revealing research, attitudes in the part of the medical profession towards the appendix have changed, and it is no longer removed routinely if not diseased. [silence] Having reviewed the positive contributions of the appendix to the human body, let’s turn now to the most common disease afflicting it, acute appendicitis. Before we review the pathophysiology, let’s take a look at a few numbers to get some idea of the frequency and prevalence of the disease.
Worldwide, acute appendicitis is one of the most common causes for both acute abdomen and emergency abdominal surgery. The United States is no exception to this prevalence, and there are approximately 300,000 cases diagnosed annually, accounting for millions of hospital days. The disease has a significant human and economic impact. In terms of prevalence, in the United States, the incidence of appendicitis peaks in the 10 to 20-year-old age group, and is about one and a half times more common in males than females. Now on to the pathophysiology of acute appendicitis.[silence] For many years, the accepted view has been that acute appendicitis is always caused by obstruction of the appendiceal lumen.
Let’s examine how that works. As mentioned previously, there is a constant production of mucus within the appendix, which ultimately flows out of it at its junction with the cecum. If the appendiceal lumen becomes obstructed, and this most commonly occurs due to a small hard piece of stool known as fecalith, the mucus secretions have no outlet and will build up within the appendiceal lumen. Pressure builds up within the appendiceal lumen causing swelling, which triggers an inflammatory reaction within the wall of the appendix.
[pause 00:12:23]
This is simple acute appendicitis. By simple, I mean inflammation of the appendix without perforation. [silence] It’s important to note that obstruction of the appendiceal lumen may occur from other sources. In addition to fecaliths, obstruction may be caused by tumors, either benign or malignant, infectious processes, especially those virally related, which may cause obstruction by triggering lymph node enlargement in the area of the appendix. Calculi , which precipitate from calcium salts contained in the appendiceal mucus, this is a fairly rare cause of obstruction. Finally lymphoid hyperplasia, swelling of the collections of lymphoid tissue contained in the appendiceal wall, as depicted earlier in this presentation.
Like lymph node enlargement, lymphoid hyperplasia may occur as a response to an infectious agent such as a virus. Many experts feel that lymphoid hyperplasia is the most common cause of luminal obstruction in the young, whereas the first four causes are more likely to occur in older patients. Now, let’s take a look at the clinical presentation of acute appendicitis. In terms of symptoms, the number one presenting symptom in acute appendicitis is abdominal pain. In my experience of 35 years of clinical work, both in family practice and urgent care, I never saw a patient who was subsequently diagnosed with acute appendicitis who did not complain of abdominal pain. The classic presentation is that of migratory pain.
Because the appendix shares nervous pathways with the mid-abdominal viscera and because these pathways lack somatic pain fibers, the onset of symptoms may be a vague discomfort in the mid-abdominal periumbilical region. At this stage, patients will often describe the symptoms to a mild case of indigestion. Within hours, as the appendiceal inflammation begins to affect the overlying parietal peritoneum, the pain becomes localized in the right lower quadrant. Migratory pain is only described by about 50% to 60% of patients presenting with acute appendicitis, with the remainder presenting with right lower quadrant pain.
The quality, intensity, and location of the pain may vary considerably depending on the location of the appendiceal tip. An inflamed appendix with the tip located anteriorly will cause the classic sharp right lower quadrant pain. Whereas a retrocecal appendix may produce a dull ache. An inflamed appendix with the tip located towards the pelvis may create the sensation of pelvic pain. In the early stages of the disease, patients may have a low-grade fever up to 101 degrees Fahrenheit. Patients presenting in the 102 to 105 range are more likely to have a perforated appendix. Anorexia is common in the early stages of acute appendicitis, while nausea, vomiting, and diarrhea are less so.
Patients with an appendiceal tip lying in the pelvis may have urinary frequency, pain on urination, and rectal pain. It’s important to note that it is not at all uncommon for patients with acute appendicitis to present with abdominal pain alone. Moving on to physical findings on examination in patients with acute appendicitis, you may have already guessed that the most common finding is abdominal tenderness to palpation, and in particular, right lower quadrant tenderness over McBurney’s point. While abdominal tenderness over McBurney’s point is considered a classic finding in acute appendicitis, it may not always be present, particularly very early on in the course when the overlying parietal peritoneum has not yet been irritated by appendiceal inflammation.
The presence of rebound tenderness in the right lower quadrant, characterized by a sudden increase in pain just as the pressure of the palpating hand is released from the abdomen, is indicative of localized peritoneal inflammation and should increase suspicion for an underlying appendicitis. There is a list of other physical signs that may be present in patients with acute appendicitis. [silence] Due to tremendous variability in the sensitivity and specificity of these signs in patients with appendicitis, they have largely been replaced by more sophisticated and accurate imaging studies such as CT, ultrasound, and MRI.
These signs may still be useful as factors in the clinical suspicion for acute appendicitis in the pediatric age group, in whom accurate imaging may be difficult to perform or undesirable due to radiation levels, or in scenarios with adult patients where sophisticated imaging studies are not available. The most useful laboratory test in helping with the diagnosis of acute appendicitis is a white blood cell count. While the white blood cell count may be normal in the early stages of acute appendicitis, particularly before gangrene or perforation has occurred, values in the range of 13,000 to 15,000 white blood cells are commonly seen.
These levels will be higher in the presence of gangrene or perforation as noted. A final note on laboratory studies in patients suspected of acute appendicitis, all women of childbearing age should have a pregnancy test performed as part of the workup. This is important as it will influence the choice of a diagnostic imaging study, and it may suggest alternative diagnoses for lower abdominal pain, for example, a right-sided tubal pregnancy. Before we leave our review of clinical evaluation to discuss imaging studies, I want to mention a tool that is used by some clinicians to assess the probability of acute appendicitis.
The Alvarado score employs a constellation of symptoms, physical examination findings, and white blood cell count to assign a score to patients being evaluated for the possibility of acute appendicitis. [silence] Patients with a score of less than five are discharged. Those with the score between five and six are observed or admitted to hospital. Those with a score higher than six are sent to surgery. To my way of thinking, the Alvarado score is most useful in situations where advanced imaging is either unavailable or unfeasible for a given patient.
A summary of 42 studies reviewed by the National Institute of Health regarding the accuracy of the Alvarado system found that it accurately diagnosed or ruled out acute appendicitis in adult men, yielded inconsistent diagnostic results in children, and tended to over predict the presence of appendicitis in adult women. In my clinical experience, if a previously well patient presents with acute onset of right lower quadrant abdominal pain, and elevated white blood cell count, and a negative pregnancy test, in the absence of other clinical features suggestive of an alternative diagnosis, the next step is to get an advanced imaging study to rule out appendicitis.
In other words, in this scenario, the patient has acute appendicitis until proven otherwise. Let’s turn now to the role of imaging studies and the diagnosis of acute appendicitis. Plain film X-rays have little usefulness in the diagnosis of acute appendicitis. The one exception to this is that if the appendix has perforated, a plain film may reveal free air beneath the diaphragms. Advanced imaging studies, specifically CT, ultrasound, and MRI may all help to make the diagnosis. Let’s take a look at the pros and cons of each of these techniques. CT scan is considered the preferred technique for the diagnosis of acute appendicitis. Compared to ultrasound or MRI, CT scan has high rates of making the diagnosis in patients with acute appendicitis and is better at excluding the diagnosis in patients with a normal appendix.
The accuracy of diagnosis is improved when iodinated contrast material is given intravenously. Typically, a CT of the abdomen and pelvis is performed, and this allows for identification or exclusion of alternate causes of lower abdominal pain as well. In terms of disadvantages, CT scan delivers a significant dose of radiation to the patient, and this makes it unsuitable for pregnant women or children. Allergy to iodinated substances or impaired renal function may preclude the use of contrast material during CT. Without contrast material, the accuracy of CT is reduced but still high.
Looking now at ultrasound, ultrasound is the preferred technique for children and pregnant women. In addition, it does not require a contrast material and may be performed at the patient’s bedside. Ultrasound is far less [unintelligible 00:22:57] of human and economic resources, and maybe available in smaller centers when CT and MRI are not. The primary disadvantage of ultrasound is that its diagnostic accuracy is considerably lower than CT or MRI. This includes a reduced ability to make the diagnosis in patients with appendicitis, as well as less accuracy in locating a normal appendix when appendicitis is absent.
Finally, in order to obtain adequate images, the ultrasound transducer must be applied to the right lower quadrant under pressure, and this may be very uncomfortable for some patients. Magnetic resonance imaging or MRI is the final imaging technique we’re going to be looking at. Like ultrasound, MRI delivers no radiation to the patient. It is suitable for pregnant women and older children who can follow instructions to remain motionless throughout the exam. Also, like ultrasound, no iodinated contrast is necessary to perform the MRI, although contrast may be used if the initial study is non-diagnostic. Unlike ultrasound, the diagnostic accuracy of MRI is comparable to CT.
Disadvantages of MRI scans and acute appendicitis include the fact that patients must remain motionless for up to 10 minutes while the scan is completed. This may be particularly challenging for small children and patients with high levels of pain. As depicted here, patients must be positioned within the relatively narrow tube of the MRI scanner, which may prove difficult for those with a tendency towards claustrophobia. Finally, because MRI is used so much less frequently than CT in most centers in the diagnosis of acute appendicitis, a lack of experience may result in greater variability in diagnostic accuracy.
A list of conditions which can mimic or approximate the symptoms of lower abdominal pain with acute appendicitis is fairly extensive and varies depending on age and gender. For example, intussusception of the bowel may cause lower abdominal pain in children less than two years of age, whereas a right-sided tubal pregnancy may occur in females of childbearing age. Rather than go into an extensive review of each of the possible differentials, I have included a link on this video page to a very concise British Medical Journal review of the alternative diagnoses. [silence]
So far, we’ve discussed the pathophysiology of simple appendicitis, that is where the appendix is inflamed but still intact. If the process is allowed to continue, the pressure within the appendiceal lumen continues to rise. Looking at a close up cross sectional view of the appendix, obstructed mucus is present in the appendiceal lumen, and the mucosa and appendiceal wall are inflamed. Retention of mucus and inflammation both contribute to increased intraluminal pressure resulting in compression of the mucosa and appendiceal wall. The vascular structures responsible for bringing oxygen and nutrients to the mucosa and wall are also compressed. This results in ischemia, a critical loss of blood flow.
The appendiceal wall undergoes necrosis, tissue death, resulting in a perforation. [silence] After the onset of abdominal symptoms, time to perforation is quite variable. Only about 15% of individuals perforate within 24 hours after onset of symptoms, with about 70% of patients perforating greater than 48 hours after onset. Once the appendiceal a wall has been breached, bacteria laden fecal material flows into the abdominal cavity. Within hours, an abscess or an inflammatory mass known as a phlegmon, may develop. Both an abscess or a phlegmon will contain the perforation and prevent the spread of infection into the peritoneal cavity.
Less commonly, neither an abscess nor a phlegmon will form resulting in a free perforation of the appendix. Infection may then spread into the peritoneal cavity causing inflammation of both the peritoneal membrane and the organs that it encloses. This is known as acute peritonitis. If left untreated, acute peritonitis can progress to septicemia, shock, and cardiovascular collapse. The final aspect of acute appendicitis we’re going to look at is treatment. For decades, surgical removal of the appendix was the gold standard for treating acute appendicitis. However, in the last many years, research data has shown that conservative non-surgical management or delayed surgical management of acute appendicitis leads to better outcomes in certain patient populations.
In addition, surgical treatment itself has changed with the advent of laparoscopic appendectomy. To date, there have been a fairly large number of studies comparing patient outcomes in surgical versus non-surgical or delayed surgical treatment as well as the laparoscopic approach compared to the more traditional open surgery. For the purposes of this presentation, I’m going to give you a fairly concise summary of the findings of these comparisons. Let’s start by considering patients with simple acute appendicitis, that is without appendiceal perforation. Most studies have found that non-surgical conservative treatment of simple acute appendicitis with intravenous and then oral antibiotics has yielded comparable outcomes to those patients treated surgically.
A significant benefit for the conservatively treated patients is that they avoid the risks associated with surgery and general anesthesia. One caveat for non-surgically treated patients is that approximately 20% to 30% of them end up requiring appendectomy within one to two years after initial treatment. In summary, initial conservative treatment of simple acute appendicitis appears to be a reasonable alternative for those patients who wish to avoid surgery if possible or for those who have other medical issues which may increase the risk of undergoing surgery and anesthesia.
Let’s take a look now at patients with acute appendicitis who have a perforation with the formation of a localized abscess. In other words, where infection has been contained within an abscess around the area of appendiceal perforation. Most data has indicated that initial conservative therapy with intravenous and then oral antibiotics followed by so-called interval appendectomy once the abscess has resolved results in fewer hospital days and fewer surgical complications at the time of appendectomy.
[pause 00:30:57]
Once the abscess has resolved and the patient is clinically normal, some surgeons have questioned the need for the interval appendectomy. A review of the current literature indicates that most surgeons still prefer to perform an interval appendectomy within a few months of resolution of the initial episode, particularly when an obstructive fecalith was identified on initial imaging. This eliminates the possibility of a recurrent and potentially more serious episode of perforated appendicitis. Patients with free perforations of the appendix or who are unstable clinically must have emergency surgical appendectomy performed.
Most such patients will have at least the beginnings of acute peritonitis and will require extensive drainage and irrigation of the peritoneal cavity in addition to removal of the appendix. [silence] Some surgical authorities believe that initial conservative management of patients with a free perforation is reasonable if the patient’s clinical signs are stable and they have pain localized to the right lower quadrant. Study data in support of this treatment regimen is as yet lacking. To bring this presentation to a close, a quick mention of open versus laparoscopic technique for performing appendectomy in acute appendicitis.
In the early days of the development of the technique, laparoscopic surgery was reserved for cases of simple acute appendicitis. With ever increasing sophistication of the technology and more experienced surgeons, the laparoscopic technique is now used in all forms of acute appendicitis including cases of free perforation and those involving acute peritonitis. The decision as to which technique to use in a given patient is now largely up to the judgment of the surgeon. For those wishing to delve more deeply into the details of treatment of acute appendicitis, I have added several links to this web page as well as the previously mentioned link regarding differential diagnosis.
Cal Shipley M.D., copyright 2020