Hip Replacement Surgery Transcript
Hip Replacement Surgery Introduction
This is Doctor Cal Shipley with a review of total hip replacement surgery, also known as total hip arthroplasty (or THA). THA is one of the most common orthopedic procedures performed in the United States with an estimated 300,000 procedures performed annually. A British orthopedic surgeon, Sir John Charnley, is credited with the development of the first, practical, artificial hip. Let’s start by looking at the anatomy of the hip.
Anatomy of the Hip
The hip joint is known as a “ball-and-socket” joint. The ball component of the joint is contributed by the femur, commonly known as the thigh bone. The spherically shaped head of the femur is the ball. Below the head is the neck of the femur. The neck is a common location for traumatic fractures of the hip. Below the neck lies the shaft of the femur which extends all the way down to the knee. The head of the femur is covered by a layer of cartilage. The socket of the hip joint is contributed by the pelvis.
A recessed area of the pelvis known as the acetabulum provides the socket. Like the head of the femur, the acetabulum is also lined by a layer of cartilage. A cross-sectional view of the acetabulum allows for a demonstration of the critical role that cartilage plays in the operation of the joint. The cartilages of the acetabulum and the femoral head provide a smooth, frictionless surface for articulation of the joint. Now that we’ve familiarized ourselves with the hip anatomy, let’s move on to the THA procedure itself.
Hip Replacement Surgery Indications
The most common indication for the THA procedure is pain and disability resulting from deterioration of the hip joint. The term deterioration typically refers specifically to a significant loss of joint cartilage on either, or both, of the acetabulum and femoral head. As demonstrated here, the loss of cartilage results in bone on bone contact between the femoral head and the acetabulum,. This results in extreme friction during articulation of the joint which causes inflammation and pain, particularly when the joint is under more stress during weight-bearing activities. This sets up a vicious cycle whereby ongoing inflammation contributes to further deterioration of the joint which increases inflammation, etc., etc. The deterioration of joint cartilage may have many causes but by far, the most common is osteoarthritis.
It is important to note that the presence of pain is not essential in candidates for THA if the degree of disability resulting from hip deterioration is interfering with activities of daily life. Finally, THA is not a minor surgical procedure and carries risk. Individuals with arthritis of the hip should always undergo a proper course of conservative, non-surgical therapy prior to consideration for the procedure.
Hip Replacement Surgery Procedure
While there are different techniques and approaches preferred by different surgeons, the goal of all THA procedures is replacement of the diseased acetabulum and femoral head with artificial components. For the purposes of this review, I am going to depict the so-called anterior approach whereby the hip joint is entered from the front of the patient. One advantage of the anterior approach is that it does not require detachment of any of the muscles around the hip joint. Some studies indicate that this approach is associated with a more rapid recovery and a reduced chance of dislocations postoperatively.
Dislocation of the Femoral Head
Irrespective of the specific approach taken by the surgeon, the next step is to dislocate the head of the femur in order to permit access to the acetabulum. The diseased cartilage in the acetabulum is then removed and the bone of the acetabulum is surgically prepared for placement of an artificial socket. The artificial socket is then inserted. Typically, the socket consists of two components, a hemispherical porous metal shell which lies in direct contact with the acetabular bone and a polyethylene inner liner designed to articulate with a highly polished, artificial, femoral head.
Hip Replacement Artificial Components
The artificial sockets come in a variety of sizes and the surgeon will choose one that provides the best fit with the acetabulum. In the past, the most common method of affixing the outer shell to the acetabular bone was with cement, but in recent years, a cementless form of outer shell has been utilized with better long-term fixation results, especially in younger patients with good bone stock. These cementless shells are made of a porous material which allows the patient’s bone to grow into, and form, a bond with the shell.
In addition, many cementless shells are coated with a chemical such as hydroxyapatite which stimulates bone growth. Once the acetabular component has been successfully fitted, the surgeon then turns his attention to the femoral head. The head and neck of the femur are removed. The structure of the femoral shaft consists of a hard outer layer of cortical bone and a soft inner layer of cancellous bone. As we will see, this multi-layered structure is the key to insertion and fixation of the femoral implant.
The femoral component consists of a detachable head typically made of cobalt, chrome, a collar, and a stem. As with the acetabular component, the currently preferred form of hip implant is cementless. The shaft is made of a porous material and may be coated with a bone stimulating compounds such as hydroxyapatite to allow for a biological fixation between the implant and the femur.
Broaches
As with the acetabular component, a cementless, femoral implant requires a healthy, thick layer of cortical bone, and may not be appropriate for older patients. To help with initial fixation and stability, the stem of a cementless implant typically has a rough, corrugated surface. Prior to insertion of the femoral component, the surgeon uses a series of devices called broaches to create a channel in the soft, cancellous bone of the femoral shaft and to determine which size femoral implant will be ideal for the patient.
The broaches are numbered corresponding to size and each broach is wider, longer, and deeper than the previous size. Each of these sizes also corresponds exactly to the same size of hip implant. The creation of the channel in the cancellous bone begins with the smallest broach. The surgeon attaches a handle to the broach. A view from above reveals the relationship between the broach, the cancellous, and the cortical bone of the femoral shaft.
Broach Insertion
Using a surgical mallet, the surgeon gently inserts the broach into the cancellous bone. Once the broach is fully inserted, the surgeon assesses it for fit using a number of criteria. On visual inspection, there should be no gap between the edge of the broach and the inner edge of the cortical bone. This image indicates the ideal situation with the edge of the broach meeting the inner aspect of the cortical bone. In addition, if there is a significant gap between the broach and the inner aspect of the cortical bone the surgeon will be able to rotate the broach as depicted here. Once the ideal broach size has been inserted there will be little or no rotational instability noted by the surgeon.
Another criteria that may be used by the surgeon to determine broach fits is leakage of cancellous fluid. The cancellous bone contains a high proportion of fluid, including the bone marrow. Compression of the cancellous bone by a fully inserted broach will squeeze fluid out into the gap between the edge of the broach and the cortical bone. In the presence of an ideally sized broach, the gap between the broach and the cortical bone is eliminated and the amount of cancellous fluid leakage observed by the surgeon is much reduced.
Implant Insertion
Finally, many surgeons perceive a “solid” feeling when the edges of an ideally sized broach meet the inner cortex of the femoral shaft upon full insertion. In order to satisfy the criteria previously mentioned and determine an ideal implant size, the surgeon inserts progressively larger broaches. Once the ideal broach size has been determined, let’s say a size 11 for purposes of this example, a correspondingly sized hip implant may be inserted into the channel created by the broach.
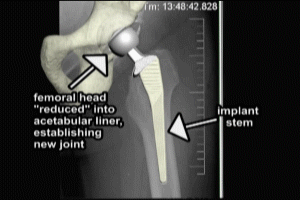
When fully inserted, the collar of the implant rests on top of the cortical bone. The edges at the top of the stem are in full contact with the inner edge of the femoral cortex. The femoral head is then attached, typically by a threaded mechanism. The new femoral head is then reduced into the liner of the acetabular component. The new hip joint is complete. X-rays may be taken while the patient is still in the operating room to determine that the new implant is in proper position.
Cal Shipley, M.D. copyright 2021